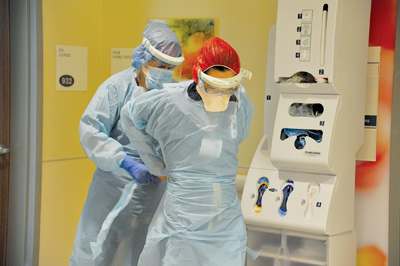
Health-Care Workers: The New First Responders of 2020
Seemingly overnight, health-care professionals became heroes all over the world. For many of us, they already were among our heroes. But with the COVID-19 pandemic bearing down on the United States and the North Bay, attention has been laser-focused on our hospitals, the workers who keep them going, and how the next few weeks will look for this vital service in our communities.
In early March, many of us didn’t know what a ventilator was, or how critical it could be to life. Now we hear daily accounts of how many or how few of these expensive machines are available in hospitals to help some of the sickest patients with coronavirus, who may be attached to one for weeks. The number needed is staggering; that there may not be enough to cover the needs of the nation is sobering.
As politicians point fingers and assign blame for a nationwide lack of basic health-care necessities and personal protective equipment (PPE), COVID patients––and others needing urgent or emergency care for other reasons––keep arriving at our hospitals.
Do health-care workers in the North Bay have enough PPE to get through the worst of the surge in patients? How are non-COVID patients receiving care, such as women about to deliver babies and cancer patients who require timely tests and treatments? The public has lots of questions for their medical providers, and the answers are changing frequently.
Testing and elective surgery
When asked about COVID-19 testing, Frank Beirne, regional chief operating officer for St. Joseph Health Northern California, said that as of early April, patients at its facilities in the North Bay (Santa Rosa Memorial Hospital, Petaluma Valley Hospital, and Queen of the Valley Hospital in Napa) have specimens collected to be submitted to labs for testing. “We collect the specimens and the testing is currently done at public health laboratories or certain qualified high-complexity labs. If a patient meets certain medical criteria suggestive of COVID-19, such as signs of a serious lower respiratory illness, we will work with our local health authorities to approve a test at an authorized site.

“This process has proven cumbersome, and efforts are underway across state and federal governments, the Centers for Disease Control and Prevention (CDC), and health-care organizations to test more people, faster,” adds Beirne. “In our experience, turnaround times have been consistently improving as more testing options become available. Getting tested and receiving the results does take time—sometimes under 24 hours, sometimes days—but our goal is to obtain results as quickly as possible.”
St. Joseph Health Medical Group also set up two “pop-up” respiratory clinics, one in Napa and a mobile clinic in Sonoma. Patients who call a St. Joseph Health Medical Group provider with respiratory issues or symptoms consistent with COVID-19 are screened for mild, moderate or acute symptoms, using County Public Health and CDC guidelines. Based on the screening, patients may be referred and scheduled for an appointment to be further evaluated. Patients scheduled for an appointment at the respiratory clinic will not necessarily be tested for COVID-19. However, the clinic has the ability to perform drive-by testing for patients who meet criteria and have appointments.
Non-coronavirus patients who were waiting on elective surgeries before the crisis, and for procedures such as routine mammograms and colonoscopies, will have to wait a little longer. “In alignment with the American College of Surgeons recommendation to review all elective surgery and invasive procedures, our hospitals decided to cancel all elective inpatient and outpatient procedures in late March,” says Beirne. “This helped to preserve capacity to meet the acute health-care needs of our patients and also minimizes the use of essential items needed to care for patients, including but not limited to, Intensive Care beds, PPE, terminal cleaning supplies, and ventilators.
We continue to closely follow the guidance offered by the state and public health officials as we begin to thoughtfully and safely reopen our hospitals to essential procedures for patients in Sonoma and Napa Counties,” Beirne adds. “We will continue to test and treat patients with COVID-19 using the best practices, safety protocols and protective equipment, as we have over past months. From the very beginning of our response to COVID-19, we have developed and implemented safety protocols to ensure the safety of our patients, providers and employees.”
Finding more PPE
As increased worldwide demand for PPE continues, hospitals across the nation are facing a shortage of crucial medical supplies to keep providers and caregivers safe. “Providence St. Joseph Health’s supply chain team has been working tirelessly to obtain PPE by every means possible, including placing large orders with suppliers and applying for supplies from the National Emergency Stockpile,” says Beirne.
“We are focusing on securing new PPE and conserving existing PPE. We are exhausting every resource available to find PPE and have implemented conservation efforts, including accepting new and unopened donations of PPE (such as N95 masks) from organizations and companies. These masks are inspected and evaluated before being deployed. We are implementing an extended use and reuse of supplies, such as N95 masks and face shields, when appropriate, following guidelines set by the CDC.”
Beirne adds that Providence St. Joseph Health is also working with Medline Industries, a medical supplies manufacturer and distributor, to reprocess procedural/surgical masks and N95 masks in its facilities using methods that are “well established and approved” by the Food and Drug Administration. “These measures use recognized filtration and testing standards for safety and help to protect every caregiver, so they can care for our patients and communities,” says Beirne. “And we are very thankful to all the local businesses, individuals, and to the state of California for their donations.”

Sutter Health is pursuing additional avenues to bolster and conserve supplies, so it can meet critical community needs while maintaining patient and frontline staff safety. “Sutter Health and Sutter Santa Rosa will continue to collaborate with local, state, and federal partners, and leverage our integrated network to deploy resources to address this continually evolving situation,” says Dan Peterson, chief executive officer of Sutter Santa Rosa Regional Hospital. “Sutter Santa Rosa staff currently have adequate PPE in accordance with CDC guidelines. It’s important that we continue to build our reserves in anticipation of a potential patient surge, so continued donations are appreciated.”
Community effort
When news reports began circulating about an impending shortage of PPE, particularly masks, Jesse Rael, M.D., stepped up to help. A radiologist with Sutter Santa Rosa, he reached out to local media in March to announce that he was accepting donations of masks, which could be dropped off in a special box in his front yard. Rael hoped that his grassroots model of gathering supplies could be rolled out in other communities. News of his effort that appeared in the Press Democrat and on KSRO Radio were enough to mobilize others to get on board.
“The majority of donations I received [arrived] in sealed packages, brand new and with the boxes intact,” says Rael. “Some boxes were opened, with one or two masks missing, but I accepted those, too. I also received some protective gowns, gloves and beautiful masks that were handmade by many in our community. I delivered masks and other protective items to our hospitals. While collecting, I soon realized how extensive the need was with many health-related people needing PPE outside of hospitals such as EMTs, medical transporters, medical clinics, chiropractors, nursing home staff and dentists. I was just glad to be of some help to our community.”

Woodworker Steve Westerman is used to having a box of N95 masks around the house. The project manager for Keysight saw the newspaper blurb about Dr. Rael’s drive for donations and it snowballed from there. He donated his personal stash of 19 individually-wrapped N95s, then reached out to friends and coworkers for their possible donations. Word reached the executive team at Keysight, and Westerman and his marketing friends started thinking bigger, he says.
He began communicating with Keysight management about spreading the word more effectively, and a flier was designed. Keysight agreed to pay for the printing costs for the first run of 5,000 fliers, which Westerman planned to distribute to grocery stores.
“Keysight has a long tradition of community support,” says Westerman. “I was overwhelmed that they responded to the effort so quickly.” Keysight also dropped off a shipment of PPE from the company’s own stock to the Sonoma County Emergency Operations Center, he says. “I believe it was several thousand masks.”
Fliers and posters
In Marin County, Mill Valley resident Linda emailed Rael because she had some extra masks, but didn’t know where to drop them off for hospitals in Marin. “I originally thought about accepting mask donations in my garage, but decided it was better if the equipment went directly to the hospitals,” says Crouse, a partner and director of marketing at BAR Architects in San Francisco.
In early March, she says, some of the hospitals hadn’t yet thought about the logistics for drop-off points for donated PPE, but she eventually received the appropriate information. She then produced 1,200 fliers and several posters with that information and distributed them to retail stores in Marin, as well as on various social media platforms. “Mollie Stones in Sausalito said they would put the fliers into customers’ grocery bags,” she says.
Santa Rosa-based Pine Creek Properties, which owns and manages numerous apartment buildings in Sonoma County, also pitched in to help after owner Kenny Martin read about Rael in the newspaper.
“I donated 2,000 N95 masks that I had purchased just a month earlier, in preparation for what was about to be thrust upon us. Our company has a staff of more than 20 who deal with the public and tenants. We can social distance out in the field, so I kept a few masks back for our workers who may be faced with a special situation, or if we have a known COVID-19 case in one of our properties. As much as I wanted to prepare my own staff for this crisis, I wanted to help out those on the front lines first.
“The crazy part is,” Martin muses, “how could a schmo like me get 2,000 N95 masks, while hospitals are having trouble finding enough?”
Hospital turned factory
At Queen of the Valley in Napa, some medical staff members were busy in early April making face shields for their colleagues, and St. Joseph Health hospitals across Northern California. California’s Office of Emergency Services delivered 5,000 face shields to the Queen in late March, but a team of eight employees decided to also construct their own, in the event the hospital runs low. Face shields protect caregivers from the forehead on down past the mouth, and are worn over masks. They offer additional protection against flying respiratory droplets, such as from coughs and sneezes that can transmit COVID-19.
Led by Mike Smith, a manager in the physical therapy department, and Jim Casciani, a retired engineer with work experience in respiratory care medical products, the hospital created an assembly line to make face shields on site. In total, the team produced 1,300 shields, using off-the-shelf materials such as marine-grade vinyl, industrial tape, foam, and elastic. Some of the supplies were purchased at craft stores and hardware stores.
After they were produced, the face shields were inspected and approved by infection prevention specialists and clinical leaders. “These face shields will safely protect our caregivers, so they can effectively care for our patients and communities,” says Gianna Peralta, infection prevention manager. “We know that to care for our patients, we must ensure the health and safety of caregivers.”
Staying calm, carrying on
Even in the midst of a pandemic, life still carries on. Sutter hospitals have implemented mandatory temperature and symptom screenings as well as face masks for all patients, visitors and staff upon entry. Additional precautions for pregnant women are also in place. Babies are still being delivered, urgent cancer patients are also being accommodated, with chemotherapy and radiation treatments also moving forward. Sutter Santa Rosa’s outpatient infusion center is still operational and actively seeing patients, according to Peterson.
Though cautiously optimistic about the coronavirus locally, Pine Creek’s Martin says he had a low point over the past few weeks. “I put up posters about practicing proper hand-washing hygiene to fight coronavirus in the common areas of our complexes. Many were then defaced or ripped off the walls. I wasn’t making a political statement. I was trying to protect our tenants. If a large part of this population are still nonbelievers, we could be in for a lot of trouble.”
A common refrain being heard again and again during this pandemic is “we’re all in this together.” An unprecedented outpouring of volunteer help, such as the home sewers crafting masks day in and day out, has shown us what we can do to feel less helpless while using our stay-at-home time productively for the greater good. Lessons learned from this crisis will stay with us all as we move forward together.
By Jean Saylor Doppenberg